The U.S. Preventive Services Task Force (USPSTF) recommends that women aged 65 and older be screened routinely for osteoporosis. The USPSTF recommends that routine screening begin at age 60 for women at increased risk for osteoporotic fractures (Go to Clinical Considerations for discussion of women at increased risk)..
Furthermore, how do you screen for osteoporosis?
The most commonly used bone measurement test used to screen for osteoporosis is central DXA; other screening tests include peripheral DXA and quantitative ultrasound (QUS). Central DXA measures BMD at the hip and lumbar spine.
Additionally, what is considered severe osteoporosis? Osteoporosis. Bone density is 2.5 SD or more below the young adult mean (−2.5 SD or lower). Severe (established) osteoporosis. Bone density is more than 2.5 SD below the young adult mean, and there have been one or more osteoporotic fractures.
Simply so, how often do you screen for osteoporosis?
Experts recommend that older women have regular bone density tests to screen for osteoporosis. But it's been unclear how often to repeat the tests. A study of nearly 5,000 women now reports that patients with healthy bone density on their first test might safely wait 15 years before getting rescreened.
What is normal bone density?
According to the World Health Organization (WHO): A T-score of -1.0 or above is normal bone density. Examples are 0.9, 0 and -0.9. A T-score between -1.0 and -2.5 means you have low bone density or osteopenia.
Related Question Answers
Can osteoporosis be reversed?
A decrease in bone density is a natural part of aging, but healthy living can slow down and even reverse bone loss. According to the National Osteoporosis Foundation, one in two women and up to one in four men will break a bone in their lifetime due to osteoporosis.Can osteoporosis be detected by a blood test?
Blood tests that may be ordered include: Blood calcium levels - this test is usually normal in osteoporosis but may be elevated with other bone diseases. Vitamin D - deficiencies can lead to decreased calcium absorption. Thyroid tests - such as T4 and TSH to screen for thyroid disease.What Is an osteoporosis screening?
Osteoporosis (Bone Density) Screening. Osteoporosis screening (often referred to as a bone density test) is conducted by using a specialized ultrasound to measure the density of the shinbone, indicating if bone density is lower than normal. This ultrasound is painless and non-invasive.What does T score and Z score mean?
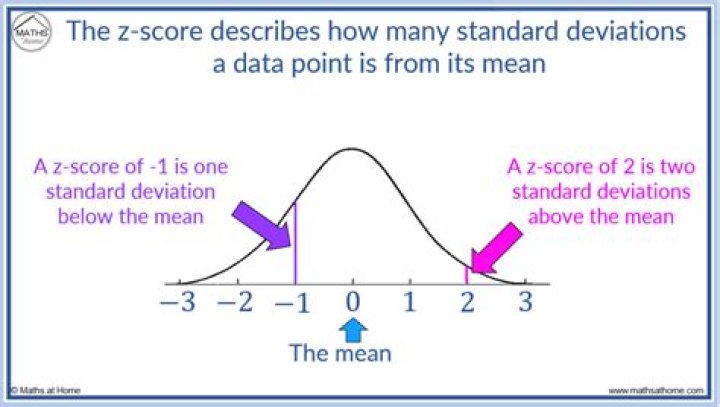
The T-score is a comparison of a person's bone density with that of a healthy 30-year-old of the same sex. The Z-score is a comparison of a person's bone density with that of an average person of the same age and sex.What tests are done to diagnose osteoporosis?
To diagnose osteoporosis and assess your risk of fracture and determine your need for treatment, your doctor will most likely order a bone density scan. This exam is used to measure bone mineral density (BMD). It is most commonly performed using dual-energy x-ray absorptiometry (DXA or DEXA) or bone densitometry.What age do you stop screening for osteoporosis?
Age to Stop Osteoporosis Screening In women aged 70 to 80 years at baseline, osteoporosis treatment is effective and mass BMD screening has been assessed as more cost-effective than no screening or screening only in women with at least one risk factor for fracture [13, 57–60].What is the life expectancy of a person with osteoporosis?
Despite reports that people with osteoporosis have an increased risk of dying prematurely, a new study has found that life expectancy of newly diagnosed and treated osteoporosis patients is in excess of 15 years in women below the age of 75 and in men below the age of 60.Can you rebuild bone density?
Healthy lifestyle choices such as proper diet, exercise, and medications can help prevent further bone loss and reduce the risk of fractures. But, lifestyle changes may not be enough if you have lost a lot of bone density. Some will slow your bone loss, and others can help rebuild bone.What is the first sign of osteoporosis?
There typically are no symptoms in the early stages of bone loss. But once your bones have been weakened by osteoporosis, you might have signs and symptoms that include: Back pain, caused by a fractured or collapsed vertebra. Loss of height over time.How long does it take for osteopenia to turn into osteoporosis?
Osteopenia is when your bones are weaker than normal but not so far gone that they break easily, which is the hallmark of osteoporosis. Your bones are usually at their densest when you're about 30. Osteopenia, if it happens at all, usually occurs after age 50.Is osteoporosis genetic?
Osteoporosis is a common disease with a strong genetic component characterised by low bone mass, microarchitectural deterioration of bone tissue and an increased risk of fracture. It is only on rare occasions that osteoporosis occurs as the result of mutations in a single gene.What should my bone mass be for my age?
Your bone density is then compared to the average BMD of an adult of your sex and race at the age of peak bone mass (approximately age 25 to 30). The result is your T score. A T score of -1 to +1 is considered normal bone density. A T score of -1 to -2.5 indicates osteopenia (low bone density).Does osteopenia always lead to osteoporosis?
If you have osteopenia, you have lower bone density than normal. Your bone density peaks when you're about 35 years old. People who have osteopenia have a lower BMD than normal, but it's not a disease. However, having osteopenia does increase your chances of developing osteoporosis.Who should have a DEXA scan?
Who should get a bone-density scan? For women over 65 and men over 70, DEXA scans are only appropriate for those with moderate risk of fracture or when the results will change the patients care plan. Younger women and men ages 50 to 69 should consider the test if they have risk factors for serious bone loss.How much does a bone density scan cost?
A DEXA scan costs about $125. And if your doctor prescribes a drug when you only have mild bone loss, you spend money you don't need to. A month's supply of generic alendronate can cost as much as $75.What is the ICD 10 code for screening for osteoporosis?
Encounter for screening for osteoporosis Z13. 820 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2020 edition of ICD-10-CM Z13. 820 became effective on October 1, 2019.Who is at risk for osteoporosis?
Women over the age of 50 are the most likely people to develop osteoporosis. The condition is 4 times as likely in women than men. Women's lighter, thinner bones and longer life spans are part of the reason they have a higher risk. Men can get osteoporosis, too -- it's just less common.How quickly does osteoporosis progress?
For women, bone loss is fastest in the first few years after menopause, but it continues gradually into the postmenopausal years. As bone density loss occurs, osteoporosis can develop. This process is slower by 10 years in men.How bad can osteoporosis get?
Severe osteoporosis Without appropriate treatment, osteoporosis can worsen. As bones get thinner and weaker, the risk of fracture increases. Symptoms of severe osteoporosis can include a fracture from a fall or even from a strong sneeze or cough. They can also include back or neck pain, or loss of height.