.
Moreover, what causes Enterobacter infections?
The source of infection may be endogenous (via colonization of the skin, gastrointestinal tract, or urinary tract) or exogenous, resulting from the ubiquitous nature of Enterobacter species.
Also, how do you treat Enterobacter aerogenes? The antimicrobials most commonly indicated in Enterobacter infections include carbapenems, fourth-generation cephalosporins, aminoglycosides, fluoroquinolones, and TMP-SMZ. Carbapenems continue to have the best activity against E cloacae, E aerogenes, and other Enterobacter species.
Beside this, is Enterobacter aerogenes dangerous?
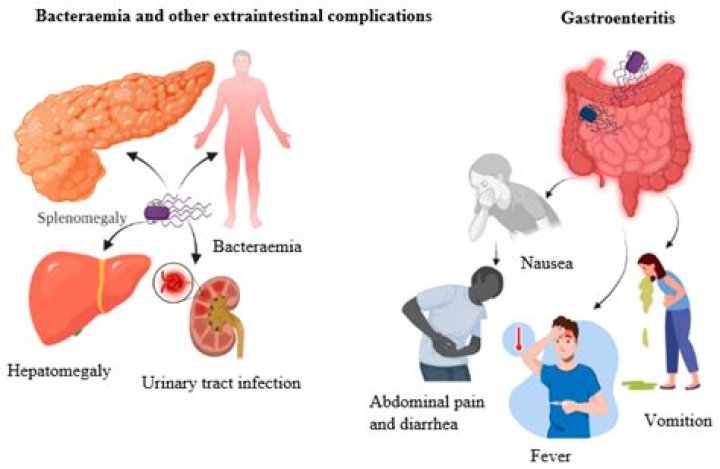
Enterobacter aerogenes is a nosocomial and pathogenic bacterium that causes opportunistic infections. It is a gram-negative, rod-shaped bacteria. E. aerogenes is generally found in the human gastrointestinal tract and does not generally cause disease in healthy individuals.
What does Enterobacter mean?
Enterobacter are gram-negative bacteria that are classified as facultative anaerobes, which means that they are able to thrive in both aerobic and anaerobic environments. Enterobacter is named for the organisms' predominant natural habitat, the intestines of animals (from Greek enteron, meaning “intestine”).
Related Question AnswersHow is Enterobacter transmitted?
Transmission and Disease Enterobacter cloacae can be acquired through the skin, urinary tract, or gastrointestinal tract. Nosocomial infection, meaning the contraction of the germ from being hospitalized, is the most prevalent mode of transmission for this organism.How do you get Enterobacter?
Enterobacter strains commonly arise from the endogenous intestinal flora of hospitalized patients but can occur in common source outbreaks or are spread from patient to patient. Infections are especially common in patients who have received antimicrobial therapy and in those in intensive care units. Enterobacter spp.How does Enterobacter cause UTI?
Pyelonephritis with or without bacteremia, prostatitis, cystitis, and asymptomatic bacteriuria can be caused by Enterobacter species, as with Escherichia coli and other gram-negative bacilli. Most Enterobacter UTIs are nosocomial and are associated with indwelling urinary catheters and/or prior antibiotic therapy.How serious is Enterobacter cloacae?
Elisabeth Presterl: Well, generally enterobacter cloacae is part of the human intestinal system. It's quite normal, but if it gets into the blood it can cause sepsis; other infections would be urinary blood infections and these are more common.What are the signs and symptoms of Enterobacter cloacae?
Enterobacter lower respiratory tract infections can manifest identically to those caused by S pneumoniae or other organisms. The physical examination findings may include apprehension, high fever or hypothermia, tachycardia, hypoxemia, tachypnea, and cyanosis.Is Enterobacter cloacae the same as E coli?
All Enterobacter species are found in water, sewage, soil, and vegetables. Enterobacter cloacae is the most frequently isolated Enterobacter species from humans and animals. Its role as an enteric pathogen has not been demonstrated. Enterobacter cloacae is less susceptible to chlorination than Escherichia coli.What does Enterobacter cloacae cause?
Enterobacter cloacae are responsible for various infections such as bacteremia, lower respiratory tract infections, skin and soft tissue infections, urinary tract infections, endocarditis, intra-abdominal infections, septic arthritis, osteomyelitis, and ophthalmic infections.Where does Enterobacter cloacae complex come from?
Enterobacter cloacae is ubiquitous in terrestrial and aquatic environments (water, sewage, soil, and food). The species occurs as commensal microflora in the intestinal tracts of humans and animals and is also pathogens in plants and insects.What is a gram negative infection?
Gram-negative bacteria cause infections including pneumonia, bloodstream infections, wound or surgical site infections, and meningitis in healthcare settings. Gram-negative infections include those caused by Klebsiella, Acinetobacter, Pseudomonas aeruginosa, and E. coli., as well as many other less common bacteria.How do you test for Enterobacter aerogenes?
The next method used was a Urea test. This test consisted of stirring the bacterial growth into a tube of phenol red and urea to test for the presence of acid. After incubation the broth was still a yellow color, giving a negative result. This confirmed that Enterobacter aerogenes was the gram-negative bacterium.Where are Enterobacter aerogenes found naturally?
Enterobacter are found in the soil, water, dairy products, and in the intestines of animals as well as humans. They are most frequently found in the gastrointestinal tract and are studied in clinical sites in stool samples.How many species of Klebsiella are there?
Three speciesIs Enterobacter cloacae complex contagious?
How is Enterobacter cloacae transmitted? Immunocompromised Patients are at risk if they come into direct or indirect contact with contaminated persons or objects. The pathogens can also be transmitted via contaminated infusion solutions or blood products.Where is Klebsiella aerogenes found?
K. aerogenes is generally found in the human gastrointestinal tract and does not generally cause disease in healthy individuals. It has been found to live in various wastes, hygienic chemicals, and soil.What antibiotics are carbapenems?
Carbapenems- Doribax.
- doripenem.
- ertapenem.
- imipenem/cilastatin.
- imipenem/cilastatin/relebactam.
- Invanz.
- meropenem.
- meropenem/vaborbactam.