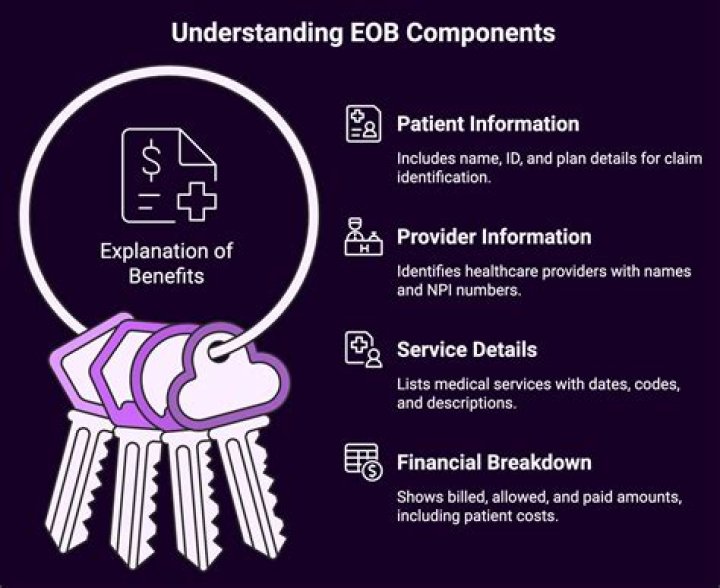
PI (Payer Initiated Reductions) is used by payers when it is believed the adjustment is not the responsibility of the patient but there is no supporting contract between the provider and payer..
Furthermore, what is Pi in billing?
Principal Investigator (PI) Responsibilities. The PI is responsible for ensuring that the IDE or the no charge device is properly set up in the facility charge master to allow accurate and compliant charging for that device before any billing will occur.
One may also ask, what is a remark code on an EOB? Remittance Advice Remark Codes (RARCs) are used to provide additional explanation for an adjustment already described by a Claim Adjustment Reason Code (CARC) or to convey information about remittance processing. Each RARC identifies a specific message as shown in the Remittance Advice Remark Code List.
Also question is, what does OA mean on an EOB?
Other Adjustments
What does PR 96 mean?
Whenever claim denied as CO 96 – Non Covered Charges it may be because of following reasons: Diagnosis or service (CPT) performed or billed are not covered based on the LCD. Services not covered due to patient current benefit plan.
Related Question Answers
What does PR 187 mean?
PR 187: Patient responsibility – consumer spending account payments (includes, but is not limited to, flexible spending account, health savings account, health reimbursement account, etc.)What does PR 27 mean?
PR-27: Expenses incurred after coverage terminated. • Claim Adjustment Reason Code (CARC) 26: Expenses incurred prior to coverage.What does OA 121 mean?
A4: OA-121 has to do with an outstanding balance owed by the patient.What is PI 204?
CARC. The claim adjustment reason code (CARC) is a code that indicates the reasons that the payer made the adjustment or denial. If the payer does not report a CARC on the ERA, this indicates that no adjustment was made. DOS (Date of Service) The date on which the medical service was provided.What does PI mean in healthcare?
principal investigator
What does PR 119 mean?
Denial Reason, Reason/Remark Code(s) PR-119: Benefit maximum for this time period or occurrence has been met.What is denial code Co 97?
It means the Evaluation and management services that are related to the surgery performed during the post-operative period will be denied as CO 97 – The benefit for this service is included in the payment or allowance for another service or procedure that has already been adjudicated.What is Reason Code 97?
Code. Description. Reason Code: 97. The benefit for this service is included in the payment/allowance for another service/procedure that has already been adjudicated. Note: Refer to the 835 Healthcare Policy Identification Segment (loop 2110 Service Payment Information REF), if present.What does code 23 mean?
Infectious disease
What is co45?
Title (optional) May 25th, 2012 - re: what is the meaning of CO-45 : Charge exceeds fee schedule/maximum allowable or contracted/legislated fee arrangement. It means it is the facility's contractual obiligation and patient can not be billed for that amount. It should be adjusted off the patient's bill.What are reasons codes?
Reason codes, also called score factors or adverse action codes, are numerical or word-based codes that describe the reasons why a particular credit score is not higher. The codes are often provided with credit score reports, or with adverse action reports issued after denial of credit.What is PR 45 in medical billing?
For example a PR-45 defines a balance after the insurance payment or adjustment that exceeds the allowed payment from the insurance carrier and assigns that balance as the patient's responsibility. CARC 97 identifies that the service billed is part of another service already paid.What is a Claim Adjustment Reason Code?
Claim Adjustment Reason Codes • X12 External Code Source 139. LAST UPDATED 11/1/2019. These codes communicate a reason for a payment adjustment that describes why a claim or service line was paid differently than it was billed.What is a status code in medical billing?
CLAIM STATUS CODES. A national administrative code set that identifies the status of health care claims. This code set is used in the X12N 277 Claim Status Inquiry and Response transaction, and is maintained by the Health Care Code Maintenance Committee.What is Medicare adjustment code CO 237?
For negative MIPS payment adjustments, the following codes will be displayed: Group Code: CO. This group code is used when a contractual agreement between the payer and payee, or a regulatory requirement, resulted in an adjustment. Claims Adjustment Reason Code (CARC) 237: “Legislated/Regulatory Penalty.What does denial code co16 mean?
The CO16 denial code alerts you that there is information that is missing in order for Medicare to process the claim. Due to the CO (Contractual Obligation) Group Code, the omitted information is the responsibility of the provider and, therefore, the patient cannot be billed for these claims.What is PR 242 denial code?
Reason and action for the denial PR 242: 245 Provider performance program withhold. 246 This non-payable code is for required reporting only. 247 Deductible for Professional service rendered in an Institutional setting and billed on an Institutional claim.What are non covered services?
A service can be considered a non-covered service for many different reasons. Services that are not considered to be medically reasonable to the patient's condition and reported diagnosis will not be covered.