.
Keeping this in view, why is sterile technique important?
Proper aseptic technique prevents contamination of cultures from foreign bacteria inherent in the environment. In addition, aseptic technique is of utmost importance to maintain pure stock cultures while transferring cultures to new media.
Also Know, what are sterile precautions? Sterile means free from germs. When you care for your catheter or surgery wound, you need to take steps to avoid spreading germs. Some cleaning and care procedures need to be done in a sterile way so that you do not get an infection. Follow your health care provider's instructions on using sterile technique.
Moreover, when was sterile technique first used?
The modern concept of asepsis evolved in the 19th century. Ignaz Semmelweis showed that hand washing prior to delivery reduced puerperal fever. After the suggestion by Louis Pasteur, Joseph Lister, 1st Baron Lister introduced the use of carbolic acid as an antiseptic, and in doing so, reduced surgical infection rates.
How is a sterile field created?
Creating and maintaining a sterile field is an essential component of aseptic technique. A sterile field is an area created by placing sterile surgical drapes around the patient's surgical site and on the stand that will hold sterile instruments and other items needed during surgery.
Related Question AnswersWhat is the sterile technique?
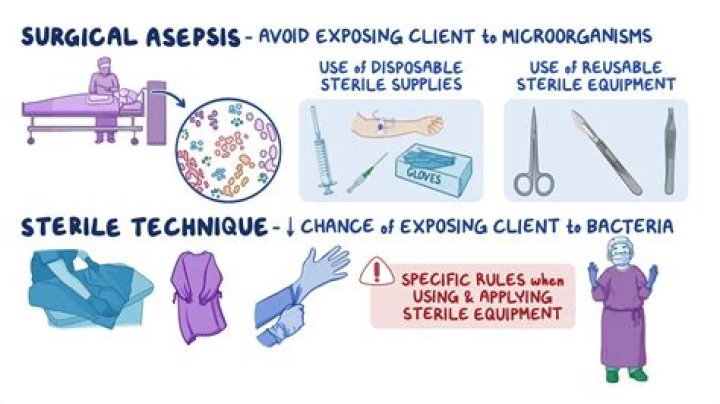
Sterile technique. Sterile is generally defined as meaning free from microorganisms. 3 Sterile technique involves strategies used in patient care to reduce exposure to microorganisms and maintain objects and areas as free from microorganisms as possible.How do you maintain sterile techniques?
10 Areas of Focus for Maintaining a Sterile Field in an ASC- Involve all team members.
- Follow the same practices every day.
- Reduce conversation in the sterile field.
- Inspect instruments and trays for tears.
- Include a sterilization indicator with each item/tray.
- Be sure before using an item.
- Face the sterile field at all times.
What are sterile items?
The Sterile Processing Department (Central Supply, or Sterile Supply as it is also known), comprises that service within the hospital in which medical/surgical supplies and equipment, both sterile and, are cleaned, prepared, processed, stored, and issued for patient care.What does sterile mean in medical terms?
adjective. The definition of sterile is something totally clean and free from bacteria, a living thing that is not able to reproduce sexually and create offspring, or something that is lacking in interest or vitality. A hospital room that has been prepped for surgery is an example of a room that is sterile.Who invented sterile technique?
Joseph ListerAre operating rooms sterile?
Keeping operating rooms clean and sterile is a vital process, and one that is constantly being tweaked. “Neither operating rooms nor storage areas will be sterile, so they need to be kept as clean as possible with regular cleaning regimes, filtered air-conditioning and restricted access,” Garcia says.What is a sterile culture?
The definition of sterile is 'completely clean, sanitized, and free of all forms of life'. Obviously you still want your cells and/or any other organisms you are studying to live, but any reagents or equipment that are used for tissue culture should be sterile.Which direction do you open a sterile package?
Sterile gloves have outer packaging that must be removed prior to starting the procedure of applying sterile gloves. 8. Open sterile packaging by peeling open the top seam and pulling down. Open sterile packaging without contaminating inner package.What is asepsis technique?
Aseptic technique means using practices and procedures to prevent contamination from pathogens. It involves applying the strictest rules to minimize the risk of infection. Healthcare workers use aseptic technique in surgery rooms, clinics, outpatient care centers, and other health care settings.Who discovered germ theory?
Louis PasteurWhat was the first antiseptic?
Lister successfully introduced carbolic acid (now known as phenol) to sterilise surgical instruments and to clean wounds. Applying Louis Pasteur's advances in microbiology, Lister championed the use of carbolic acid as an antiseptic, so that it became the first widely used antiseptic in surgery.What are the two types of asepsis?
There are two types of asepsis medical and surgical. practices that reduce the dumber, growth, transfer and spread of pathogenic microorganisms. They include hand washing, bathing, cleaning environment, gloving, gowning, wearing mask, hair and shoe covers, disinfecting articles and use of antiseptics.Who is the father of sterilization?
Joseph ListerWhat is an example of asepsis?
So cleaning up spills, dirty surfaces and using disinfectant would be examples of this. Medical asepsis also includes the use of PPE (personal protective equipment), like gloves, gowns, and even masks, eye and face shields.How do you achieve asepsis?
Patient and equipment preparation Aseptic preparation may involve: disinfecting a patient's skin using antiseptic wipes. sterilizing equipment and instruments before a procedure. keeping sterilized instruments inside plastic wrappers to prevent contamination before use.How surgeons wash their hands?
Wash hands and arms with anitmicrobial soap. Scrub each side of each finger, between the fingers, and the back and front of the hand for two minutes. Proceed to scrub the arms, keeping the hand higher than the arm at all times. This prevents bacteria-laden soap and water from contaminating the hand.What does it mean to sterilize someone?
to destroy microorganisms in or on, usually by bringing to a high temperature with steam, dry heat, or boiling liquid. to destroy the ability of (a person or animal) to reproduce by removing the sex organs or inhibiting their functions. to make (land) barren or unproductive.What are the 5 standard precautions for infection control?
Infection Control and Prevention - Standard Precautions- Standard Precautions.
- Hand Hygiene.
- Personal Protective Equipment (PPE)
- Needlestick and Sharps Injury Prevention.
- Cleaning and Disinfection.
- Respiratory Hygiene (Cough Etiquette)
- Waste Disposal.
- Safe Injection Practices.